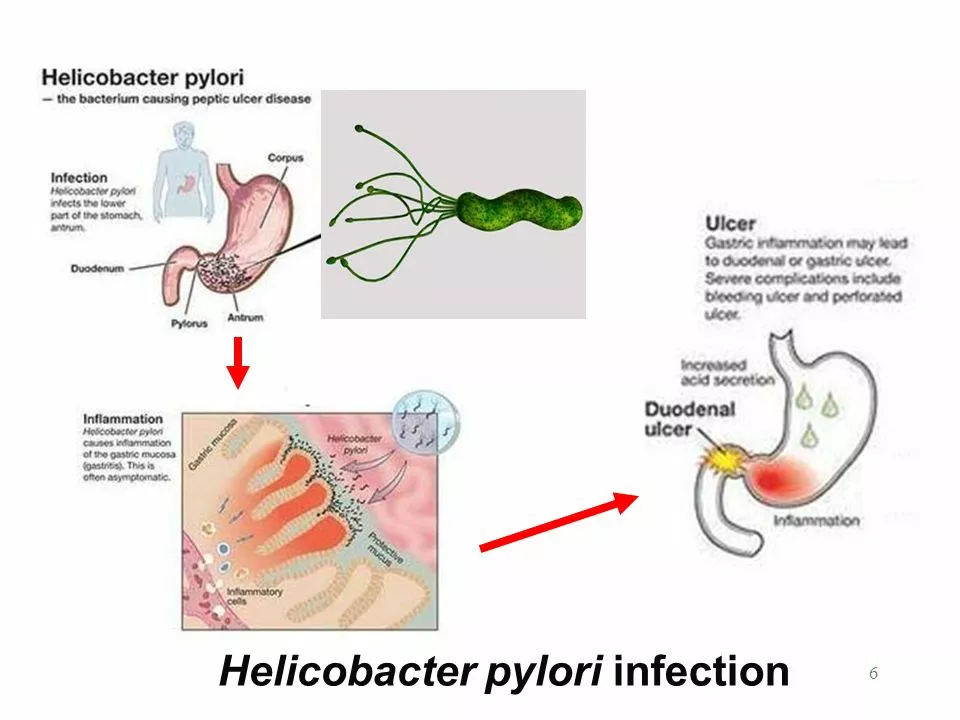
Helicobacter pylori: causes, symptoms and treatment
If you've heard of H. pylori, you probably know it's linked to stomach pain and ulcers. H. pylori (short for Helicobacter pylori) is a common bacteria that lives in the stomach lining. Not everyone who has it gets sick, but when it does cause trouble, the results can be painful and persistent.
Why it matters: H. pylori can cause gastritis (stomach inflammation), peptic ulcers, and in rare long-term cases it raises the risk of stomach cancer. The good news is that most infections respond to treatment if they’re caught early.
Symptoms to watch for
Symptoms are not the same for everyone. Common signs include a burning or aching pain in the upper belly, bloating, burping, nausea, and loss of appetite. If you notice black or tarry stools, bloody vomit, unexplained weight loss, or severe abdominal pain, get medical help right away—those can signal a serious ulcer or bleeding.
How doctors diagnose H. pylori
There are a few reliable tests. The urea breath test is quick and accurate: you drink a harmless liquid and breathe into a bag so the lab can check for the bacteria. Stool antigen tests detect H. pylori proteins in a poop sample. If you’re getting an endoscopy for other reasons, a biopsy from the stomach lining can be tested directly.
Blood antibody tests exist but aren’t used as often because they can’t tell if an infection is current or happened in the past. Your doctor will pick the best test based on your symptoms and medical history.
Treatment usually involves a short course of antibiotics plus an acid reducer (a proton pump inhibitor) to help heal the lining. Because H. pylori has growing antibiotic resistance in some areas, your doctor might choose medications based on local resistance patterns or previous antibiotic use.
Common regimens include two antibiotics (like amoxicillin, clarithromycin, or metronidazole) plus a PPI. When resistance is suspected, a bismuth quadruple therapy (bismuth, tetracycline, metronidazole, plus a PPI) is a solid option.
After treatment, doctors usually re-test—commonly with a breath or stool test—to confirm the bacteria are gone. If symptoms return, further testing or a different antibiotic plan may be needed.
Practical tips: finish the full antibiotic course, avoid NSAIDs (they can worsen ulcers), and talk to your doctor about side effects. If you’re buying medication online, use verified pharmacies and keep a record of prescriptions and lot numbers.
Related reading on this site covers antibiotic choices, resistance trends, and safe online pharmacy tips—useful if you want deeper info on drugs and buying medication safely. If you’re worried about symptoms, see a healthcare provider. Quick diagnosis and the right treatment usually fix the problem and stop complications from developing.