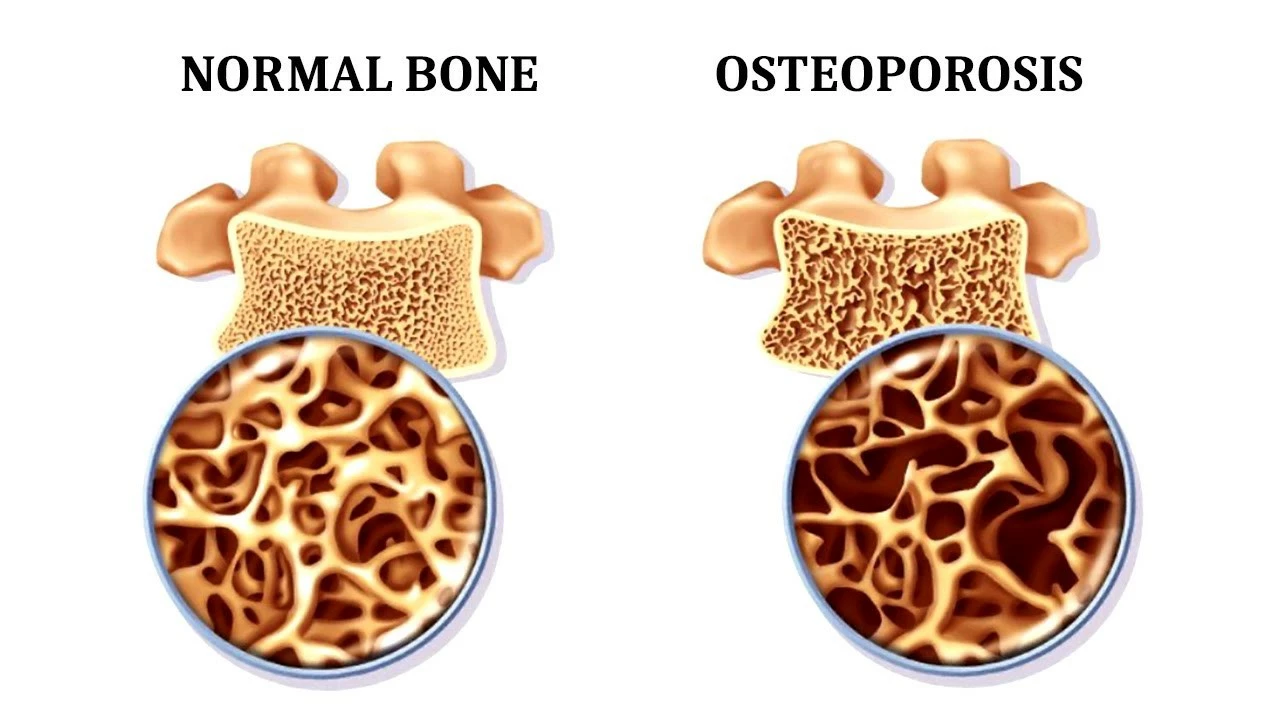
Osteoporosis: Practical Guide to Stronger Bones
Broken bones from a small fall aren’t normal. That’s often the first sign of osteoporosis — weaker bones that break more easily. If you’re worried about bone health or have a family history, this page gives straight answers you can use today.
How osteoporosis is diagnosed
Your doctor will start with risk factors: age, sex, smoking, steroid use, low body weight, early menopause, or a family history of fractures. The main test is a DEXA scan (bone density test). It’s quick, painless, and shows a T-score that tells whether you have normal bone density, low bone mass (osteopenia), or osteoporosis.
Blood tests may check calcium, vitamin D, thyroid function, and markers of bone turnover. If you’ve had a fracture from minimal trauma, that alone often triggers treatment without delay.
Simple steps to protect your bones
Move more. Weight-bearing activities—walking, jogging, stair climbing—and resistance training build bone strength. Aim for at least 2–3 sessions per week that challenge your muscles.
Eat for your bones. Get enough calcium (about 1,000–1,200 mg daily for most adults) from food first—dairy, leafy greens, fortified foods—and use supplements only if you can’t meet needs. Vitamin D helps your body absorb calcium; common doses range from 800–2,000 IU daily depending on your levels. Ask your doctor for a blood test before starting high doses.
Quit smoking and limit alcohol. Smoking speeds bone loss. Drinking more than 2–3 units per day raises fracture risk and interferes with bone repair.
Fall-proof your home. Remove loose rugs, add grab bars, improve lighting, and wear supportive shoes. Even small changes cut the chance of a dangerous fall.
Medications matter if your risk is high. First-line drugs are usually bisphosphonates (alendronate, risedronate) taken weekly or monthly. They lower fracture risk and are well-studied. Follow instructions: take on an empty stomach with a full glass of water and stay upright for 30–60 minutes to avoid irritation.
Other options include denosumab (injection every 6 months), anabolic agents like teriparatide for very low bone density, and selective estrogen receptor modulators for certain women. Hormone therapy may help around menopause but has trade-offs—talk it over with your doctor. All meds have pros and cons; treatment choice depends on fracture risk, age, and other health issues.
Keep follow-up. Bone density tests are usually repeated every 1–3 years to track response. If you’re on treatment, your doctor will watch for side effects and decide how long to continue therapy.
If you’ve broken a bone after a minor bump, or if you have multiple risk factors, see a clinician now. Early steps—exercise, nutrition, and the right tests—make a big difference in keeping you active and reducing fractures.