Parkinson's treatment: practical steps to feel better every day
Parkinson's disease affects movement, mood, and daily routines. The goal of treatment is simple: reduce symptoms, keep you independent, and slow problems that get worse over time. You’ll often combine medicines, physical therapy, lifestyle changes, and sometimes surgery. Here’s a clear, practical guide to the main options and how they fit into real life.
Medications to know
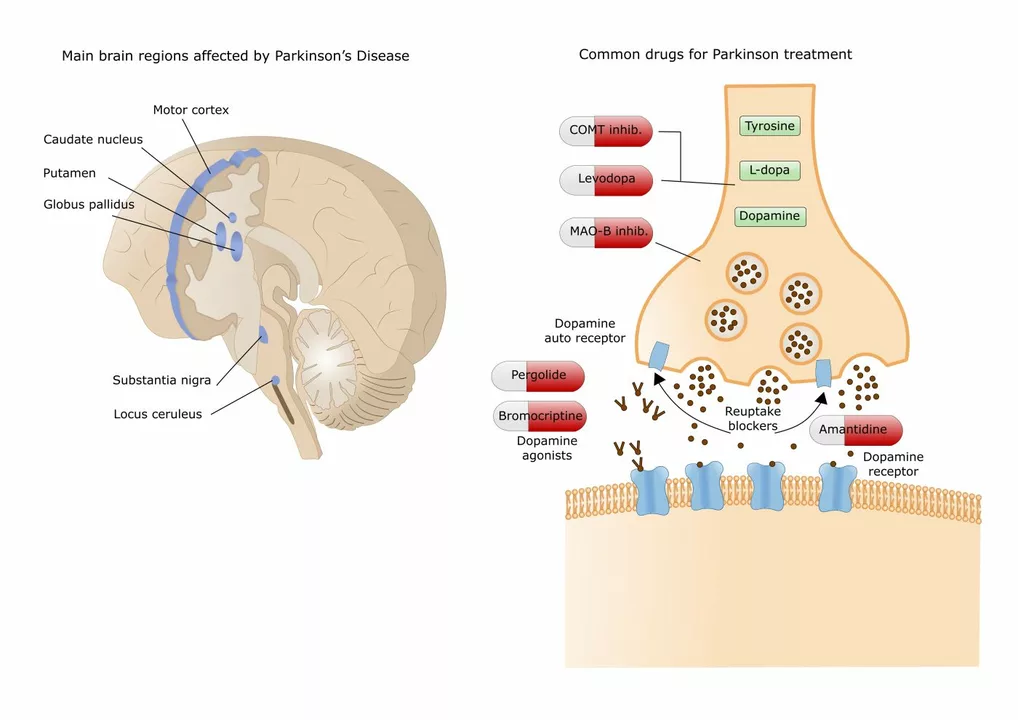
Levodopa is the most effective drug for movement symptoms. It’s usually paired with carbidopa to reduce side effects. Dopamine agonists (like pramipexole) and MAO-B inhibitors (like selegiline) help some people, especially early on. COMT inhibitors and amantadine are added when levodopa wears off or causes dyskinesia. Each drug has pros and cons—side effects can include sleepiness, confusion, or nausea—so you and your neurologist will tune doses over time.
Timing matters. Take levodopa at the same times each day and track when symptoms return. A simple notebook or a phone note about "on" and "off" times helps your doctor adjust drugs. Avoid sudden changes without medical advice; stopping some meds abruptly can cause serious problems.
Therapies and lifestyle that help
Exercise is one of the best tools. Walking, strength training, balance drills, tai chi, and cycling improve mobility and mood. Physical therapists teach targeted exercises to reduce falls and keep joints flexible. Speech therapists help with voice volume and swallowing. Occupational therapists show tricks to make dressing, eating, and writing easier.
Sleep, nutrition, and routine matter. High-protein meals can interfere with levodopa absorption; your doctor may suggest shifting protein to dinner. Good sleep hygiene and treating restless legs or sleep apnea improve daytime energy. Mental health support for anxiety or depression is important—talk therapy and some medications can help without worsening motor symptoms.
If medicines stop working well or cause severe side effects, surgical options exist. Deep brain stimulation (DBS) can cut tremors and reduce medication needs for suitable candidates. Continuous infusion therapies—like intestinal levodopa gel or apomorphine pumps—smooth out motor fluctuations for people with severe wearing-off. Not everyone is a candidate; testing and careful follow-up are required.
Small practical tips make daily life easier. Use a pill organizer and set alarms. Wear a medical ID that lists your condition and meds. Keep a simple symptom diary to share with your neurologist. Plan activities when your medication is at peak effectiveness.
Talk openly with your care team. Ask about side effects, drug interactions, and when to see a specialist. If you notice sudden worsening, balance loss, new hallucinations, or trouble swallowing, contact a doctor right away. With the right mix of meds, therapy, and daily strategies, many people with Parkinson’s keep active and enjoy good quality of life.