Stroke: Recognize Fast, Act Faster
Stroke can change a life in minutes. If you spot face droop, arm weakness, or slurred speech, call emergency services right away. Time matters: treatments work best within the first few hours.
Use the FAST check — Face, Arms, Speech, Time. Ask the person to smile, raise both arms, and repeat a simple sentence. Any sudden change is a red flag. Don’t wait to see if it gets better.
While waiting for help, keep the person comfortable and awake if possible. Loosen tight clothes, clear their airway, and note the time symptoms started. Avoid giving food, drinks, or medications unless instructed by a dispatcher.
What happens at the hospital
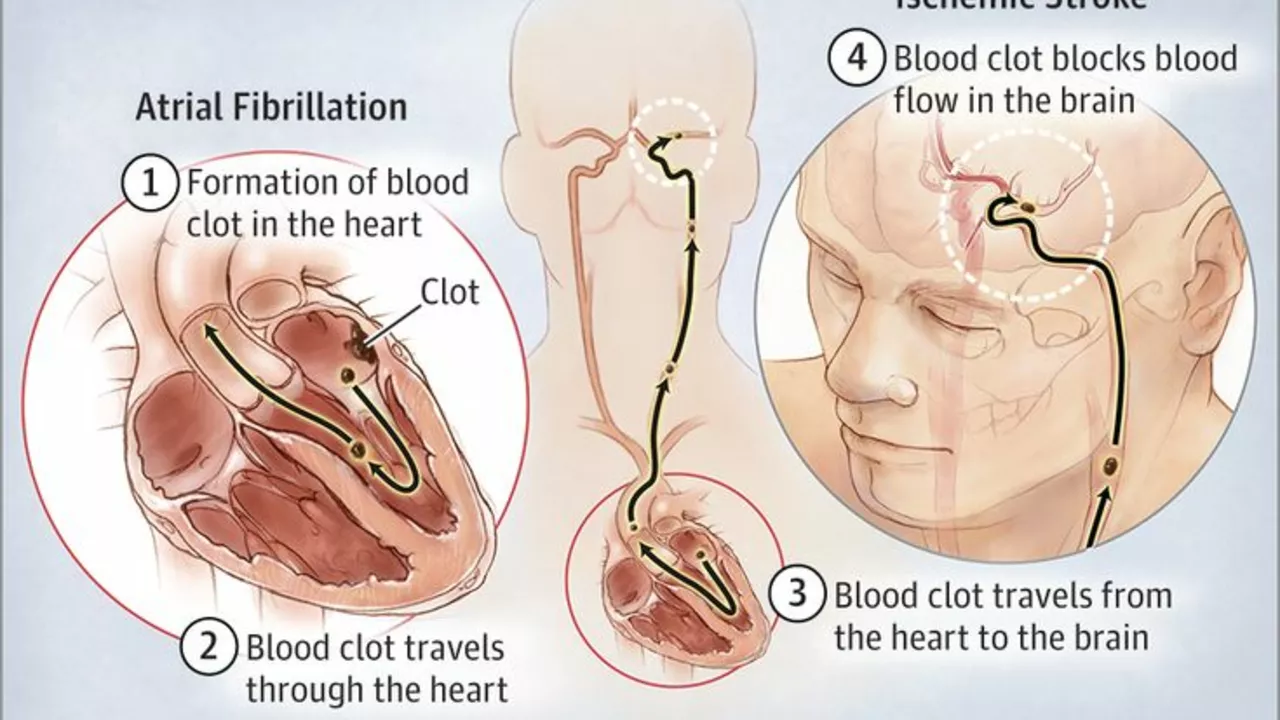
Emergency teams will do quick scans to find out if the stroke is ischemic (blockage) or hemorrhagic (bleed). For ischemic strokes, clot-busting drugs or mechanical thrombectomy can reduce damage — but they’re time-dependent. If it’s a bleed, different treatments apply. Be ready to share medical history, medications, and the exact time symptoms began.
After the emergency: recovery and rehab
Recovery starts in the hospital and keeps going at home. Physical, speech, and occupational therapy aim to rebuild strength and skills. Small, daily goals beat huge, vague ones — focus on one task at a time, like walking to the mailbox or making a sandwich. Caregivers should build a routine that balances therapy and rest.
Medications often include blood thinners, blood pressure control, cholesterol-lowering drugs, and diabetes management. Stick to the plan your doctor gives and ask questions if something’s unclear. Lifestyle changes — quit smoking, cut back on salt, move more, and follow a heart-healthy diet — cut your risk of another stroke.
Emotional recovery matters as much as physical. Depression and anxiety are common after stroke. Talk to your care team about mental health support and join a support group where people share realistic tips. Small wins matter: celebrating them keeps motivation up.
Want practical tools? Keep a list of emergency numbers, medication doses, and allergy info near the phone. Use pill organizers, set alarms, and keep a simple calendar of appointments and therapy sessions. If mobility is an issue, ask about home modifications like grab bars, ramps, and non-slip mats.
Prevention is practical: control blood pressure, manage cholesterol, treat atrial fibrillation when present, stay active, and limit alcohol. If you smoke, get help quitting — that single change cuts stroke risk fast.
On this site you’ll find articles about medications, mental health after illness, and managing chronic conditions that link directly to stroke care. Browse our stroke tag for guides on blood thinners, rehab tips, and how to find reliable online pharmacies when you need meds.
One last tip: train family members on the FAST test and keep a written emergency plan. When stroke strikes, a prepared household can make the difference between recovery and lasting damage.
Ask your doctor clear questions: what medications and doses you need, warning signs to watch for, rehab timetable, driving restrictions, and where to find community support or financial aid programs locally available.